Just as engines all have systems to regulate the rate of fuel burning, living organisms have multiple molecular mechanisms to control how much and how fast our fuel (basically glucose and fats) is converted to usable energy for maintenance and repair of their physical structures. In the case of humans and other animals, the main “throttle” system is mediated through the actions of thyroid hormones. These hormones are constructed from the amino acid L-Tyrosine and iodine atoms.
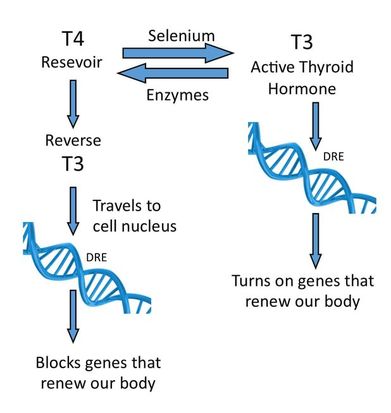
The body uses various enzymes to make four different thyroid hormones designated T1, T2, T3 and T4. The numbers indicate the number of iodine atoms attached to the basic double Tyrosine ring structures. Different selenium containing enzymes catalyze the reactions. T4, also known as L-thyroxine (brand name Synthroid) is produced about four-fold more abundantly than T3. T4 has very low biological activity and basically acts as a reservoir for the active thyroid hormone T3. The latter’s biochemical name is tri-iodothyronine. After one of the iodine atoms is cleaved from T4 to make T3, it travels to the nucleus of the cell and attaches to “DNA response elements” (DRE). This causes the gene that is controlled by the DRE to be copied (transcribed) and then the product becomes a template for the synthesis of whatever protein that segment of the DNA which stores that part of the Library of Life known as the human genome.
I am explaining this in detail so you can understand how important a healthy thyroid hormone system is to human wellbeing. Some of the genes that T3 binds to and turns on are for the synthesis of mitochondrial enzymes that produce the energy of life – ATP. T4 is converted to T3 at a faster rate when signals coming from many areas of the body’s biochemical pathways call for more energy production. For example, if we need to do a lot of physical work, more T3 is created and various genes are turned on. These genes involve energy production and regulation of virtually all body processes.
If the need for energy, DNA synthesis, hormone receptor production and a myriad of other functions decrease, conversion of T4 to T3 diminishes. If for any reason the body isn’t able to convert enough T4 to T3, all systems slow down. Of course if the person’s thyroid gland itself is sluggish or shut down completely due to autoimmunity or toxins, etc., the person has true hypothyroidism. Both T4 and T3 are reduced or absent and the person is very ill. They swell up, gain weight, have profound fatigue and eventually die. This was the natural history of hypothyroidism before the 1880’s when it was found that these patients could be helped dramatically by the use of dried extract from animal thyroid glands, mainly from swine and cows. This preparation is still available on prescription as desiccated thyroid (Armour, WP, Nature-throid, etc.).
At some point in time, a drug company peddled the idea that because T4 is converted to T3 by the body on an as needed basis, a pure, synthetic form of T4 (Synthroid = synthetic thyroid hormone T4) is all that is required for all patients. Part of the problems is that the whole biochemical understanding of T3 and T4 were not yet known. Still, doctors have been misled to believe that T4 alone is adequate and the only lab test that is used to judge whether the dose of T4 is adequate for any patient is the level of the hormone TSH (Thyroid Stimulating Hormone). This hormone is secreted by the pituitary gland when that gland senses that the thyroid hormones are too low. If the thyroid gland is functioning properly, the increased TSH causes an upregulation of T3 and T4 production. As the hormones rise, the pituitary backs off. This feedback adjustment is continuous. As a result, the “only TSH matters” paradigm, if the doctor sees that your TSH is between the laboratory “reference range” of 0.4-4.5, they pronounce the patient to be just fine. If the patient complains that they are still cold, tired, depressed, swollen and can’t lose weight, they are told it isn’t because of their thyroid dose! The truth is, the TSH range is just made up by a computer – it has nothing to do with biology and health. Many endocrinologists believe that the goal of treatment should be getting the TSH around 1.0 and certainly no higher than 2.0.
However, even if the TSH is at an ideal level, the patient may still not feel well. Remember, they might not be converting T4 to T3. We can get a measurement of Free T3 – the ultimate active thyroid hormone that binds to those DNA receptors and renews our body. In those cases, if the mixture of T3 and T4 in a desiccated thyroid extract isn’t getting the patient where they need to be, we add some pure T3 as a separate prescription. This often makes all the difference for the patient. Even though their other MD claimed that “your TSH is just fine on your dose of Synthroid,” they really needed some T3.
The plot thickens….it turns out that when a person is under a lot of stress (psychosocial, chronic infection, autoimmunity, metabolic syndrome, etc.) the body has a mechanism to force the person to slow down and conserve energy. Most of us won’t slow down until our systems shut down completely and we are diagnosed with chronic fatigue syndrome for example.
This mechanism involves T4 being converted to a separate form of T3 called Reverse T3. This hormone not only doesn’t turn on the genes which active T3 does, it actually binds the T3 receptor and blocks real T3 from having any effect! (second diagram here) The medical profession has named this phenomenon “Euthyroid sick syndrome.” They admit that the patient has all the symptoms of thyroid dysfunction, but there is nothing wrong with their thyroid biology. In these cases, one must treat the associated medical condition and often use even high doses of pure T3 at multiple times per day in order to “unlock” the T3 receptors.
Treatment of thyroid system dysfunction is by no means as simple as measuring TSH, giving Synthroid, getting the TSH between 0.4-4.5 and sending the patient out as properly treated.
There are many reasons for the array of thyroid dysfunctions: thyroid failure, problems converting T4 to T3, hyperproduction of Reverse T3, deficiency of minerals needed in thyroid hormone production, autoimmune disorders, notably adrenal gland issues.
We can measure all of the necessary parameters of your thyroid function: TSH, free T4, free T3, total T3 and reverse T3, and can then embark on bringing all of these to desirable levels. It is through coordinating the patients signs and symptoms with the lab measurements that we will be able to bring this most important component of your metabolic health into balance.
The body uses various enzymes to make four different thyroid hormones designated T1, T2, T3 and T4. The numbers indicate the number of iodine atoms attached to the basic double Tyrosine ring structures. Different selenium containing enzymes catalyze the reactions. T4, also known as L-thyroxine (brand name Synthroid) is produced about four-fold more abundantly than T3. T4 has very low biological activity and basically acts as a reservoir for the active thyroid hormone T3. The latter’s biochemical name is tri-iodothyronine. After one of the iodine atoms is cleaved from T4 to make T3, it travels to the nucleus of the cell and attaches to “DNA response elements” (DRE). This causes the gene that is controlled by the DRE to be copied (transcribed) and then the product becomes a template for the synthesis of whatever protein that segment of the DNA which stores that part of the Library of Life known as the human genome.
I am explaining this in detail so you can understand how important a healthy thyroid hormone system is to human wellbeing. Some of the genes that T3 binds to and turns on are for the synthesis of mitochondrial enzymes that produce the energy of life – ATP. T4 is converted to T3 at a faster rate when signals coming from many areas of the body’s biochemical pathways call for more energy production. For example, if we need to do a lot of physical work, more T3 is created and various genes are turned on. These genes involve energy production and regulation of virtually all body processes.
If the need for energy, DNA synthesis, hormone receptor production and a myriad of other functions decrease, conversion of T4 to T3 diminishes. If for any reason the body isn’t able to convert enough T4 to T3, all systems slow down. Of course if the person’s thyroid gland itself is sluggish or shut down completely due to autoimmunity or toxins, etc., the person has true hypothyroidism. Both T4 and T3 are reduced or absent and the person is very ill. They swell up, gain weight, have profound fatigue and eventually die. This was the natural history of hypothyroidism before the 1880’s when it was found that these patients could be helped dramatically by the use of dried extract from animal thyroid glands, mainly from swine and cows. This preparation is still available on prescription as desiccated thyroid (Armour, WP, Nature-throid, etc.).
At some point in time, a drug company peddled the idea that because T4 is converted to T3 by the body on an as needed basis, a pure, synthetic form of T4 (Synthroid = synthetic thyroid hormone T4) is all that is required for all patients. Part of the problems is that the whole biochemical understanding of T3 and T4 were not yet known. Still, doctors have been misled to believe that T4 alone is adequate and the only lab test that is used to judge whether the dose of T4 is adequate for any patient is the level of the hormone TSH (Thyroid Stimulating Hormone). This hormone is secreted by the pituitary gland when that gland senses that the thyroid hormones are too low. If the thyroid gland is functioning properly, the increased TSH causes an upregulation of T3 and T4 production. As the hormones rise, the pituitary backs off. This feedback adjustment is continuous. As a result, the “only TSH matters” paradigm, if the doctor sees that your TSH is between the laboratory “reference range” of 0.4-4.5, they pronounce the patient to be just fine. If the patient complains that they are still cold, tired, depressed, swollen and can’t lose weight, they are told it isn’t because of their thyroid dose! The truth is, the TSH range is just made up by a computer – it has nothing to do with biology and health. Many endocrinologists believe that the goal of treatment should be getting the TSH around 1.0 and certainly no higher than 2.0.
However, even if the TSH is at an ideal level, the patient may still not feel well. Remember, they might not be converting T4 to T3. We can get a measurement of Free T3 – the ultimate active thyroid hormone that binds to those DNA receptors and renews our body. In those cases, if the mixture of T3 and T4 in a desiccated thyroid extract isn’t getting the patient where they need to be, we add some pure T3 as a separate prescription. This often makes all the difference for the patient. Even though their other MD claimed that “your TSH is just fine on your dose of Synthroid,” they really needed some T3.
The plot thickens….it turns out that when a person is under a lot of stress (psychosocial, chronic infection, autoimmunity, metabolic syndrome, etc.) the body has a mechanism to force the person to slow down and conserve energy. Most of us won’t slow down until our systems shut down completely and we are diagnosed with chronic fatigue syndrome for example.
This mechanism involves T4 being converted to a separate form of T3 called Reverse T3. This hormone not only doesn’t turn on the genes which active T3 does, it actually binds the T3 receptor and blocks real T3 from having any effect! (second diagram here) The medical profession has named this phenomenon “Euthyroid sick syndrome.” They admit that the patient has all the symptoms of thyroid dysfunction, but there is nothing wrong with their thyroid biology. In these cases, one must treat the associated medical condition and often use even high doses of pure T3 at multiple times per day in order to “unlock” the T3 receptors.
Treatment of thyroid system dysfunction is by no means as simple as measuring TSH, giving Synthroid, getting the TSH between 0.4-4.5 and sending the patient out as properly treated.
There are many reasons for the array of thyroid dysfunctions: thyroid failure, problems converting T4 to T3, hyperproduction of Reverse T3, deficiency of minerals needed in thyroid hormone production, autoimmune disorders, notably adrenal gland issues.
We can measure all of the necessary parameters of your thyroid function: TSH, free T4, free T3, total T3 and reverse T3, and can then embark on bringing all of these to desirable levels. It is through coordinating the patients signs and symptoms with the lab measurements that we will be able to bring this most important component of your metabolic health into balance.

